Tag: Weight loss surgery
Mission Statement
August 14, 2014 1:15 pm
Mission Statement for Central Valley Bariatrics and Dr. Ara Keshishian “The best patient that I can have is the most knowledgeable patient”
This is one of the “lines” that I use during my teaching and consultations sessions. I firmly believe that a patients should have all the pertinent information before they decide to proceed with a treatment plan. Be the treatment is medical in nature or surgical the patient needs to have all the scientific facts before an informed decision is made.
Part of my duty is to provide the information in a scientific and concise fashion in non-medical terms. Additional resources, such as this blog, FB group (The one managed by our office, and those maintained by others) along with the Webinar hosted by us, all serve to complement each other for providing a forum for exchange of information.
The value of information exchanged between patients can not be underestimated. Patients who have walked the path can provide a much more practical experience that I can ever share with a patient. The information shared between patient can and should carry a wider range of topics. It is to be noted however, that no information exchanged between patients should replace the advice of a patients’ surgeon.
For most of us that offer weight loss surgery, we realize that there is a lot more to the care of our patients that just to “cut” and hope for the best! The best outcome is dependent as much on the follow up care as it is to the surgery itself.
I personally believe that the care should be compassionate, respectful, caring and professional. There is no reason why the advice given should include disrespectful, or otherwise demeaning comments, suggestions or innuendoes. These have always been the guiding principals based on which we will conduct our practice on the Facebook, our blog and in person. No one, be patients, my office staff or myself should tolerate any personal threats, foul language or disrespect. For those who may see values to demeaning and inflammatory discussion tones, I wish you the best in other venues.
Ara
July 2, 2014 Group Meeting Recap
July 03, 2014 7:11 am
First and foremost, We apologize for the confusion and last minute change with the webinar. It was set to go and logged in then the internet dropped the group meeting. The meeting site automatically marked the meeting as over. We sent out e-mails with the new URL for the group meeting but it took time. Thank you for your patience with this new platform. Although far reaching, it comes with downsides and hopefully we can make this a long term way to reach our patients. Lesson learned, don’t rely on wireless internet access for webinars. The Anemia slides will be added to our website dssurgery.com soon.
Ferritin is a protein that acts like your savings account. It’s like a holding tank. When you have a blood loss your body goes to Ferritin stores for iron to increase red blood cell production. Iron is like money in your pocket. For small and daily building of red blood cells. Transferrin is a protein transport that carries the iron. Copper is also needed to transport iron. Iron can be readily available but will not be utilized unless your protein levels are adequate. The protein level on laboratory studies needs to be at least 6 gm/dL & Albumin 3.2 gm/dL for adequate iron utilization. Vitamin B12 also is needed for iron utilization.
Iron metabolism in the DS patient is limited due to several factors. In unaltered anatomy Iron enters the stomach where it is exposed to acid and changes into a form which allows it to be absorbed. Then it enters the duodenum which is the chief area of the small intestines where iron absorption takes place. There is possibly a second minor site of absorption near the end of the ileum. However, after the DS there is a small portion of the duodenum that is left after the pyloric value for iron absorption. Below is a list of iron rich foods. Also remember to take Vitamin C with your iron supplements and when eating plant based iron rich foods add a food that is high in Vitamin C.
There was a brief discussion regarding Calcium oxalate kidney stones. That talk can be found on our website. Treatment is limiting oxalate containing foods and to increase calcium supplements to 3,000mg daily but to take half with food and the other half without food. Also Vitamin K2 can also decrease kidney stones.
Fissures where also briefly discussed. Fissures are most likely caused by the unopposed bile salts entering the colon after DS. Bile is alkaline and causes irritation to the mucosa. Treatment is liberal use of barrier type creams/ointments, controlling loose stools by watching if certain food items cause them or by using fiber with half the liquid mixed with it. The fiber with less liquid acts as a sponge to give more form to the stool.
We had anemia themed snacks at the live group meeting. Pate, Southwest ground Bison, and a Mayan Pumpkin seed dip. Here is the information on the nutritional value of Bison versus other meats. It is higher in iron and Vitamin B12 and lower in fat and cholesterol.
Iron Content of Common Foods
This chart shows the amount of total iron in food. Iron from most animal sources (heme iron) usually is more readily absorbed than iron from plant sources of food (non-heme iron). Include a source of vitamin C or heme iron to improve the absorption of non-heme iron.
Sources of Predominantly Heme Iron
|
FOOD
|
IRON (MILLIGRAMS)
|
|
Beef liver, braised (3 oz)
|
5.8
|
|
Lean sirloin, broiled (3 oz)
|
2.9
|
|
Lean ground beef, broiled (3 oz)
|
1.8
|
|
Skinless chicken breast, roasted dark meat (3 oz)
|
1.1
|
|
Skinless chicken breast, roasted white meat (3 oz)
|
0.9
|
|
Pork, lean, roasted (3 oz)
|
0.9
|
|
Salmon, canned with bone (3 oz)
|
0.7
|
Sources of Non-Heme Iron
|
FOOD
|
IRON (MILLIGRAMS)
|
|
Fortified breakfast cereal (1 cup)*
|
4.5 – 18
|
|
Pumpkin seeds (1 oz)
|
4.2
|
|
Blackstrap molasses (1 Tablespoon)
|
3.5
|
|
Soybean nuts (1/2 cup)
|
3.5
|
|
Bran (1/2 cup)
|
3.0
|
|
Spinach, boiled (1/2 cup)
|
3.2
|
|
Red kidney beans, cooked (1/2 cup)
|
2.6
|
|
Prune juice (3/4 cup)
|
2.3
|
|
Lima beans, cooked (1/2 cup)
|
2.2
|
|
Tofu, firm (1/2 cup)
|
2.0
|
|
Enriched rice, cooked (1/2 cup)
|
1.4
|
|
Pretzels (1 oz)
|
1.2
|
|
Whole-wheat bread (1 slice)
|
0.9
|
|
Green beans, cooked (1/2 cup)
|
0.8
|
|
White bread, made with enriched flour (1 slice)
|
0.8
|
|
Egg yolk, large (1)
|
0.6
|
|
Peanut butter, chunky (2 tablespoons)
|
0.6
|
|
Apricots, dried (3)
|
0.6
|
|
Zucchini, cooked (1/2 cup)
|
0.3
|
|
Cranberry juice (3/4 cup)
|
0.3
|
|
Unenriched rice, cooked (1/2 cup)
|
0.2
|
|
Grapes (1/3 cup)
|
0.1
|
|
Egg white, large (1)
|
From: The American Dietetic Association’s COMPLETE FOOD & NUTRITION GUIDE, 2nd ed. 2002.
USDA National Nutrient Database
Shared Success Story: Cyndi E. Had a Gastric Bypass to Duodenal Switch Revision
June 17, 2014 6:29 am
My journey to lose weight has taken most of my life. Losing weight is not just about food or eating too much, but a combination of genetics, emotions, and habits. My experience began at age 13 and has continued throughout my life. I have tried everything! I had a previous RNY Gastric Bypass, and knew something was wrong. I had seen another Bariatric surgeon who said there is nothing I can do for you because you failed. My primary Doctor asked me “does your husband love you?” Of course, but what does that have to do with me knowing there is something medically wrong with me? Again, I was brushed off and told to come back in two weeks. Leaving that day, I knew I was never going back. I went home and googled, “Bariatric Surgeon”, as I had for the past 3-4 years. Then, through a series of events was put in touch with Barbara Metcalf, a bariatric nurse, who lived in my town. As I explained my story to Barbara, she shared information with me about Duodenal Switch operation, and gave me names of two surgeons.
I contacted Dr. Ara Keshishian, in Glendale, and had a consultation that week. Meeting “Dr. K” was amazing! It was the first time a Doctor did not blame me for my weight. He explained that each weight loss surgery has different measures of success, percentages of weight loss by surgery, and outcomes. Dr K told me that I may have been a success with the RNY Gastric Bypass, based on the numbers, however it became clear that I did have complications associated with the gastric bypass. I was scheduled for an Endoscopy the next week, which Dr. K performed. The endoscopy confirmed that I had a Gastro-gastric Fistula. Simply put, this was an abnormal connection between the bypassed stomach and the small pouch created by the RNY Gastric Bypass surgery. Food could travel two ways, thus rendering the Gastric Bypass ineffective, and causing weight gain.
Dr. Keshishian performed a revision to the Duodenal Switch Surgery on May 31, 2013. This procedure corrected my anatomy, enabling me to lose weight and regain my health once again. I have had wonderful success and I have lost 104 pounds. More importantly, I do not have the complication of the dumping syndrome, episodes of nausea and vomiting and am leading a normal life. I am not prisoner to my weight, what I can and cannot eat or the fear of weight gain.
I contacted Dr. Ara Keshishian, in Glendale, and had a consultation that week. Meeting “Dr. K” was amazing! It was the first time a Doctor did not blame me for my weight. He explained that each weight loss surgery has different measures of success, percentages of weight loss by surgery, and outcomes. Dr K told me that I may have been a success with the RNY Gastric Bypass, based on the numbers, however it became clear that I did have complications associated with the gastric bypass. I was scheduled for an Endoscopy the next week, which Dr. K performed. The endoscopy confirmed that I had a Gastro-gastric Fistula. Simply put, this was an abnormal connection between the bypassed stomach and the small pouch created by the RNY Gastric Bypass surgery. Food could travel two ways, thus rendering the Gastric Bypass ineffective, and causing weight gain.
Dr. Keshishian performed a revision to the Duodenal Switch Surgery on May 31, 2013. This procedure corrected my anatomy, enabling me to lose weight and regain my health once again. I have had wonderful success and I have lost 104 pounds. More importantly, I do not have the complication of the dumping syndrome, episodes of nausea and vomiting and am leading a normal life. I am not prisoner to my weight, what I can and cannot eat or the fear of weight gain.
Sunshine, Water, Rest, Air, Exercise and Diet
May 23, 2014 4:10 pm
Sunshine, Water, Rest, Air, Exercise and Diet
Of course this is over simplified, but we can’t forget the importance of the basics in our general well being. Weight loss surgery and especially Duodenal Switch have distinctive supplement requirements that need to be individualized based on your individual needs.
Sunshine is essential to life. It provides the light that wakes us and helps to regulate wake/sleep cycles and provides us with a feeling of well being. Sunlight is not only the basis of all living things but crucial in boosting the bodies Vitamin D supply. Most Vitamin D deficiencies in the general public are caused by lack of sun exposure. It is important to note that our bodies can not accomplish Vitamin D metabolism if we are wearing sunscreen. Without adequate Vitamin D stores bones will not form properly, muscle strength is impaired and osteoporosis. Vitamin D 1,25(OH) accumulates in cell nuclei of the intestine, where it enhances calcium and phosphorus absorption, controlling the flow of calcium into and out of bones to regulate bone-calcium metabolism. However, after weight loss surgery this mechanism can be impaired. Addition supplementation of Vitamin D is usually required based on laboratory studies following weight loss surgery. Duodenal Switch patients should take a dry “water miscible” type of Vitamin D3 daily.
Water comprises 50-60% of our adult bodies. Water is essential in cell life. It aids in transporting vitamins, nutrients and minerals to our cells. Chemical and Metabolic reactions rely on water to remove waste products including toxins that the organs’ cells reject and removes them through urine and feces. Our body temperature is regulated by sweating and the evaporation of water on the skin. Also, effectively Lubricating our joints and acting as a shock absorber for our brain, eyes, and spinal cord. Decreased stomach size, after weight loss surgery, limits the amount of water a person can drink at one time. It is imperative that patients ingest enough waters and fluids after surgery. We like to see our patients consume a minimum of 64 ounces of fluids a day, more on warmer days.
Rest is something we can all use more of. Lack of sleep can cause a whole host of health issues ranging from altered levels of hormones involved in metabolism, appetite regulation, stress response to cardiovascular health, insulin resistance, immune function and most importantly post-operatively tissue repair, muscle growth and protein synthesis. It’s easy to take rest for granted but do not underestimate the power of sleep.
Air is an obvious essential of life. It is important in about every function of our cells. After surgery it is important to lung health and tissue repair. Be aware of the type of air you are breathing. Pollution and contaminants in the air can impair lung function. After surgery your breathing and breathing exercises will prevent complications such as pneumonia and atelectasis. Long term air contaminants can cause asthma and long term lung health. In addition, post surgical patients will need to use their incentive spirometers to combat lung complications.
Exercise’s health benefits can not be denied. Exercise combat health conditions and disease such as stroke, metabolic syndrome, diabetes and cardiovascular disease. It also improves emotional outlook and mood. Physical activity stimulates the brain to release chemicals that involve increasing memory function. Exercise helps maintain healthy weight, improves energy, promotes better sleep, lowers stress and anxiety. Needless, to say after surgery exercise is extremely important for all the above reasons but also to ward off complications such as pulmonary embolism and deep vein thrombosis.
Diet is last but definitely not least. Balance along with moderation and eating whole unprocessed foods are best ways to ensure your health. We derive most our building blocks for cell growth from the nutrients we consume. The quality of the food we put into our bodies is important in lowering health risks such as cardiovascular disease, cancer, and weight control. Protein is crucial in muscle growth, hemoglobin, cell structure and enzymes formation. It is extremely important after weight loss surgery to remain diligent about protein intake throughout your lifetime.
It is interesting to see how all these elements are so intertwined in their synergy to maintain health. Most are easily found or done in nature. When engaging in one of these elements, many of the others are needed or benefited by the doing the first. Exercise requires that you stay hydrated, deep breath, possibly out in the sunlight and therefore you will rest better. Always follow your surgeon’s orders and recommendations based on your individual health status and laboratory studies.
Our First Featured Success Story
May 16, 2014 9:47 am
Patricia Welborn
Iron Deficiency Anemia
May 13, 2014 8:38 am
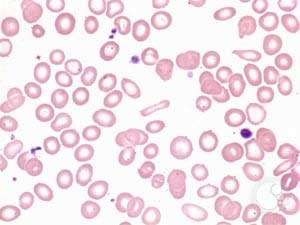
Iron Deficiency Anemia is a common problem in society and weight loss surgical patients. Anemia is usually easily treatable, although requires adequate surveillance and diligence in treatment. Microcytic/hypochromic (small pale colored red blood cells) erythrocytes indicate some inadequacy of structural matter, usually, not enough hemoglobin. This is most commonly due to an inadequate dietary supply of iron. In fact, iron deficiency anemia is the most common of all anemias.
Determining the cause of the iron deficiency is of pivotal importance in selecting appropriate therapy. Microcytic/hypochromic erythrocytes may also be seen in anemia of chronic disease, in thalassemia and in the sideroblastic anemias.
Symptoms of iron deficiency include:
- Being tired and feeling weak
- Getting frequent infections
- Feeling cold all the time
- Having swelling in the tongue
- Struggling to keep up at school or work
- Restless legs syndrome
- In children, having delayed mental development
- Feeling tired and weak
- Joint pain
- Abdominal pain
Possible Causes other than the above:
Blood loss is the most common cause of iron deficiency. Menstruation is the most likely reason in women ages 15 to 45 years. Iron deficiency anemia in adult men and postmenopausal women is most likely due to chronic gastrointestinal blood loss. Such losses are usually secondary to ulcerating lesions [peptic ulcer disease, mucosal trauma (hiatal hernias), drug ingestion (aspirin, nonsteroidal anti-inflammatory drugs, steroids, potassium), parasitic infections, inflammatory bowel disease and malignancy.
Undergoing several surgeries within a short time frame is also a source of blood loss. Frequently Duodenal Switch (DS) patients become anemic after their panniculectomy, breast reductions, arm or thigh lifts because of the short interval between operations. Also pregnancy after weight loss surgery can increase chances of developing iron deficiency anemia. After consecutive surgeries it is important to monitor your Iron, Ferritin and Transferrin, Total Iron Binding Capacity levels. Any drop in Ferritin or Transferin levels should be discussed with your DS surgeon. It is important to keep your levels with in normal limits because it can be challenging to bring these levels back up.Lack of dietary iron may cause anemia in infancy when the daily need for iron is not met by milk alone. This is why iron supplements are given to infants. Iron deficiency is a major cause of anemia in pregnancy.
Malabsorption of iron is a rare cause of iron deficiency in the general public but is seen in patients who have had a partial gastrectomy, RNY Gastric Bypass, or who have a surgical malabsorption, such as Duodenal Switch. Iron is absorbed through the duodenum and the first part of the jejunum. After DS there is only a small section (approximately 5cm) of the duodenum that comes into contact with the iron source in the GI tract. The remainder of duodenum and the jejunum after DS is now the biliopancreatic limb. There is an area of small intestine in the ileum that also absorb iron to a lesser degree in normal anatomy.
The following are definitions of Iron Deficiency Anemia diagnostic laboratory studies:
Ferritin is in essence an “iron buffer”, taking up excess iron or releasing iron as needed. Small amounts of ferritin, derived from iron stores, circulate in the plasma.
The amount of serum ferritin closely reflects iron stores, thus providing a readily measured assessment of body iron stores.
Ferritin is in essence an “iron buffer”, taking up excess iron or releasing iron as needed. Small amounts of ferritin, derived from iron stores, circulate in the plasma. The amount of serum ferritin closely reflects iron stores, thus providing a readily measured assessment of body iron stores.
-
- Transferrin, the major iron transport protein, is synthesized by the liver and macrophages (type of blood cell). Each molecule of transferrin can bind two at- oms of iron. Usually about one-third (25 – 45%) of the total transferrin is bound to iron (referred to as % saturation)Transferrin carries iron via plasma to cells throughtout the body, though the most important site of delivery is to the mar- row erythroblast. Non-heme iron (mainly Fe +++(Iron) ) is stabilized by gastric HCl; bound to mucin and then transferred to a mucosal cell surface receptor.
Most heme iron is catabolized to Fe ++ (Iron) and tetrapyrrole in the mucosal cell. In the mucosal cell the iron is bound to mobilferrin, transported through the cell to the submucosal capillary network where the iron is oxidized to Fe+++, bound to transferrin and delivered via the blood to the marrow and other tissues. Note that some iron is stored or “trapped” as ferritin in the mucosal cell. This “trapped” iron plays only a minor role in regulation of iron intake/loss as it is readily overwhelmed by ingestion of inorganic iron.
Total Iron Binding Capacity approximates a measure of transferrin. Serum iron is a measure of Fe bound to transferrin. Normally 25 – 45% of transferrin is bound to iron, ie. The % saturation of transferrin. In inflammatory and malignant conditions transferrin is decreased possibly due to macrophage degradation. Iron is decreased due to decreased release of iron from macrophages into the plasma. Iron deficiency is best screened for with serum ferritin levels (serum ferritin levels correspond to marrow stores). A serum ferritin of 12-307 ng/ml is the normal range.
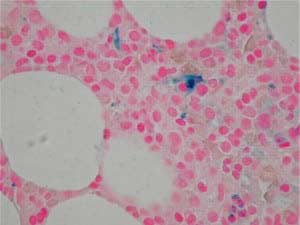
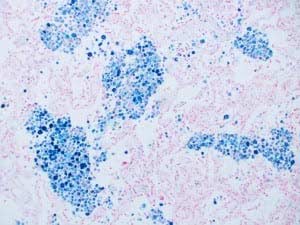
The definitive test for iron deficiency is a Prussian blue stained bone marrow. The upper image demonstrates an absence of iron in the bone marrow macro-phages of an individual with iron deficiency.
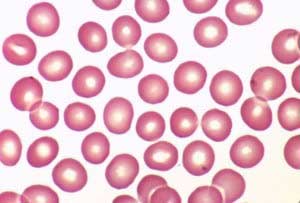
Compare the upper image with the lower image of a normal bone marrow stained with Prussian blue and demonstrating coarse granular storage iron in macrophages.
Normal Iron Ranges:
Normal results of iron testing may be different for men, women, and children. Iron and TIBC are measured in micrograms per deciliter (mcg/dL). Normal results for iron are:
- 65 to 175 mcg/dL for men
- 50 to 170 mcg/dL for women
- 50 to 120 mcg/dL for children
Normal results for TIBC are 250 to 450 mcg/dL for men and women.
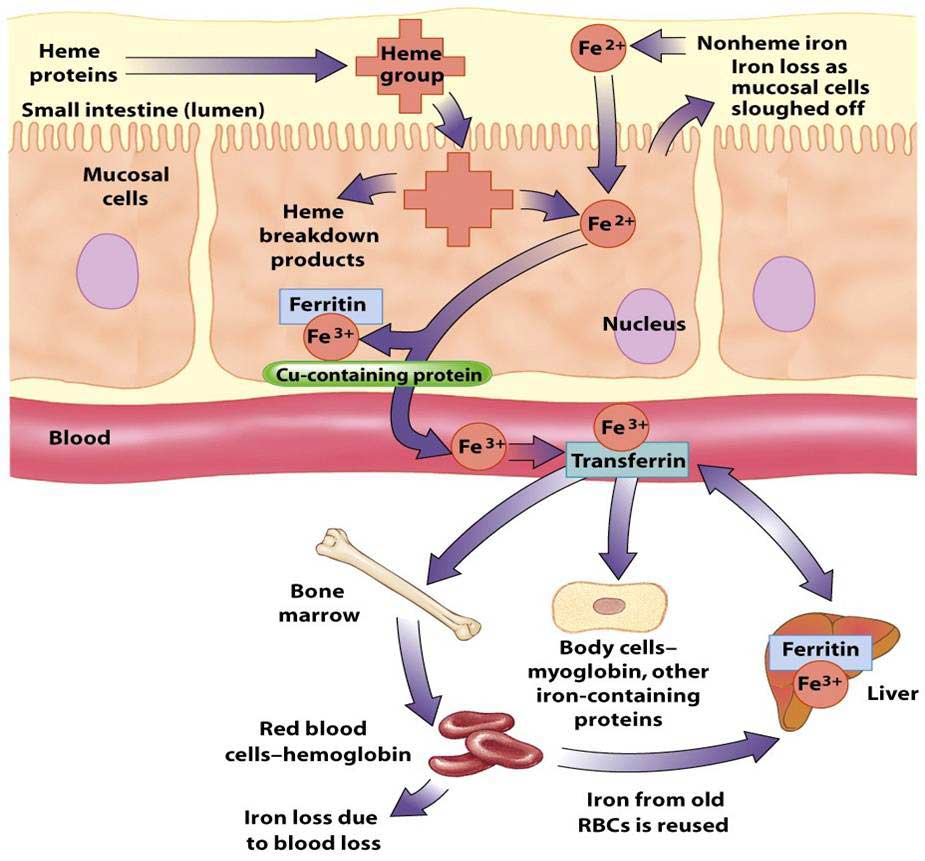
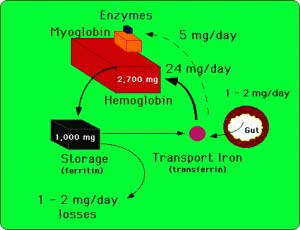
The diagram below shows the normal uptake, storage and loss of iron within the cell. An excellent explanation of iron transport physiology can be found here: https://sickle.bwh.harvard.edu/iron_transport.html
Iron is continually conserved and recycled for use in heme and non-heme enzymes. About 1 to 2 mg of iron are lost each day to sloughing of skin and mucosal cells of the gastrointestinal and genitouretal tracts. This obligate iron loss is balanced by iron absorption from the gastrointestinal tract. Only a small fraction of the 4 grams of body iron circulate as part of transferrin at any given time. Body iron is most prominently represented in hemoglobin and in ferritin.
Treatment:
There are different oral iron formulations available. I recommend heme iron instead of ferrous sulfate or ferrous fumarate. After 3 months of therapy it is necessary to repeat laboratory blood levels to determine the next course of action. Iron supplements along other medications should be stored away from children in “child proof” containers. Your pharmacist will be able to instruct you with the correct way of taking the iron supplements, and possible interference with other medications that you may be taking.
In severe anemia and/or iron deficiencies anemias resistant to oral iron supplementation, it may be necessary to have iron injections or infusions intravenously. If you have any questions please contact us either by email or phone.
In summary, iron deficiency anemia develops gradually. It also takes a great deal of time to build iron levels back up again. The importance of continued surveillance of laboratory studies is crucial after weight loss surgery. In addition, the treatment of iron deficiency anemia requires diligence in taking the iron supplement or reacting to the inability to absorb oral iron supplements by using iron infusions. Please contact our office if you have not had your yearly lab work or you may have your primary care physician order these studies.
Breaking news!
May 12, 2014 7:44 am
“Depo” Shot and Weight Gain
September 16, 2013 4:14 pm
Female patients having weight loss surgery should use two forms of Birth control for 18 months after weight loss surgery. Depo shots are suppose to prevent ovulation for a prolonged period of time. An attractive aspect of it is once a patient get the injection, there is not need to worry about birth control till the next injection is due.
There have been a number of studies that have associated Depo shots with weight gain.
Below are three citations from pubmed and the ACOG website.
Weight Gain