Category: upper GI
Bowel Obstruction After DS
August 20, 2014 12:47 am
One of the potential complications of any abdominal surgery is Bowel Obstruction. If the treating physician (usually the primary care, or the emergency room doctor) is not absolutely clear of the anatomy of a patent post duodenal Switch or the Gastric bypass surgeries this will pose a diagnostic dilemma. In intact anatomy the GI tract start at the mouth and ends up at the rectum as a long tube. After the Duodenal Switch the small bowel has two parallel limbs, the alimentary limb brings the food down from the stomach, and the biliopancreatic limb brings down the biliopancreatic secretions. These two limbs join and form the common channel.
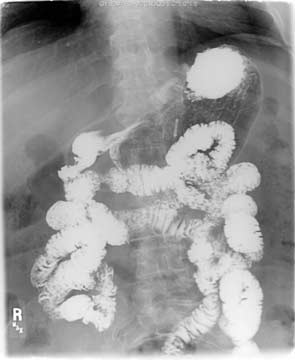
In normal anatomy, bowel obstruction may present with nausea, vomiting, abdominal cramps, inability to pass gas, and/or have bowel movements. In this case, the X-ray will also show dilated loops of bowel and if oral contrast is given with the X-ray, there will be no contrast past the obstruction. Think of it as a garden hose that has been kinked and no water is going thru.
In this upper GI- the contrast travels down the small bowel and the entire small bowel is the same caliber. This is normal study with no evidence of obstruction. In a patient with the DS, the patient my have the biliopancreaitc limb obstruction, with an identical X-ray as above, since the oral contrast given will never get to the biliopancreatic limb and it will not show if it is dilated or not.
In duodenal switch operation, a patient may have complete obstruction of the alimentary limb, with nausea, vomiting and abdominal pain, and yet have bowel movements because the content of the biliopancreatic limb is getting to the common channel. Similarly, a patient with biliopancreatic limb may have nausea, but no vomiting, because the obstructed biliopancreatic limb is not connected to the stomach and the content can’t not be expelled from the stomach.
It is critical to make sure that a patient with a suspected bowel obstruction after the DS, is evaluated with the understanding that the common signs and symptoms, and the diagnostic workup will not provide an accurate picture. A patient with the DS or RNY, can have bowel obstruction and still have bowel movement, and no vomiting.
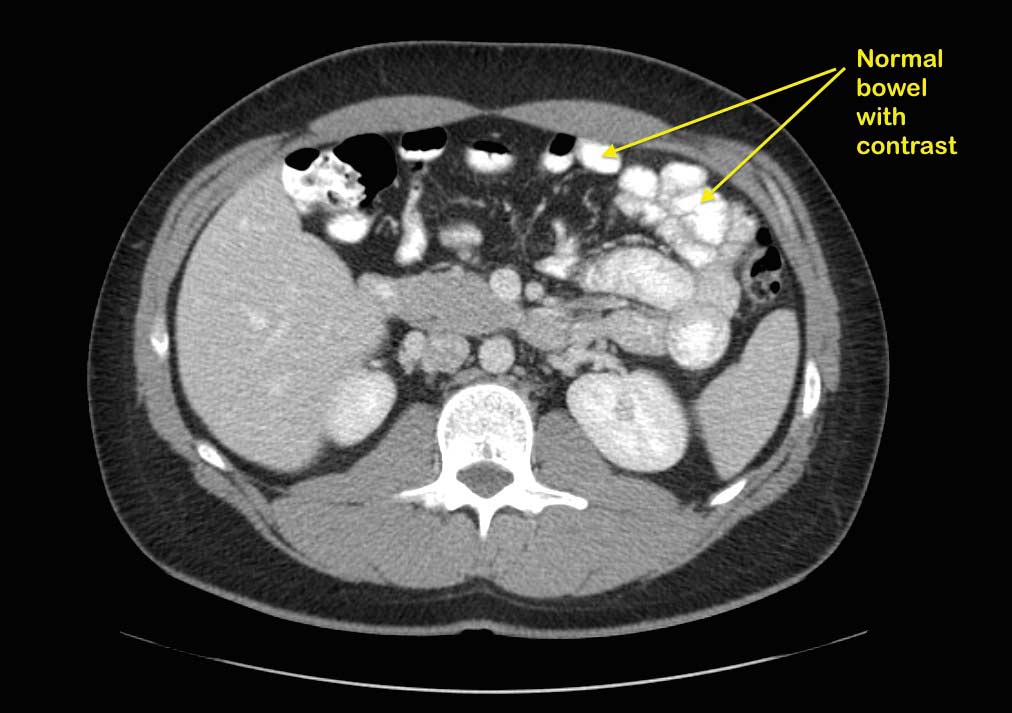
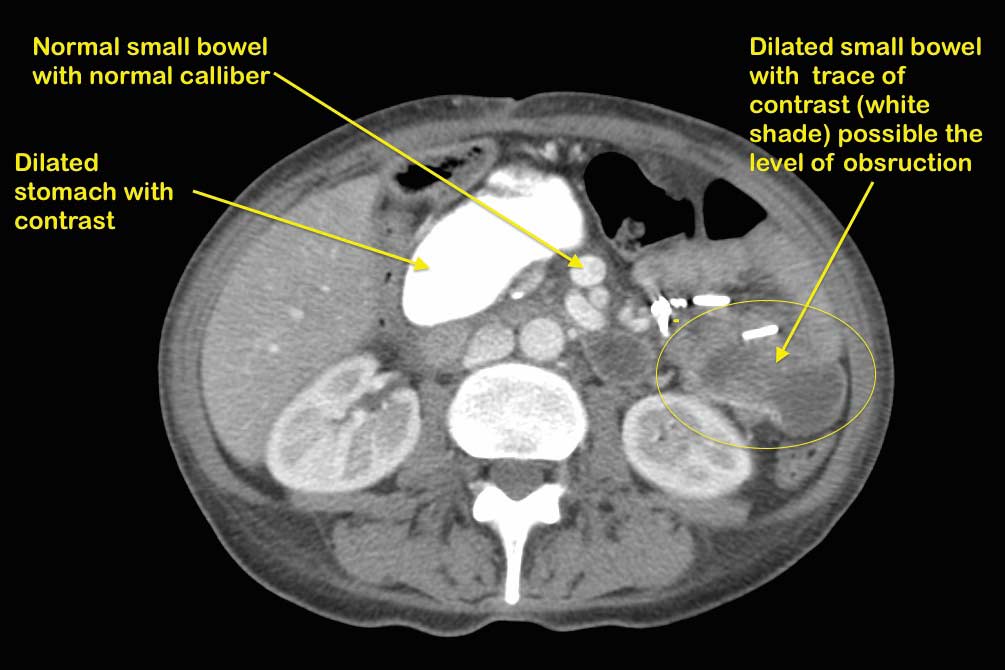
A patient with suspected bowel obstruction should have CT scan of the Abdomen with oral and IV contrast. The cardinal findings will be “dilated loops of bowel with no contrast within the lumen of the bowel”. This is highly suspicious for bowel obstruction after DS, where the regular x ray will not pick this up. Additionally, abnormal liver function test may suggest biliopancreatic limb obstruction.
Bowel Obstruction After Duodenal Switch
August 19, 2014 4:47 pm
One of the potential complications of any abdominal surgery is Bowel Obstruction. If the treating physician (usually the primary care, or the emergency room doctor) is not absolutely clear of the anatomy of a patent post duodenal Switch or the Gastric bypass surgeries this will pose a diagnostic dilemma. In intact anatomy the GI tract start at the mouth and ends up at the rectum as a long tube. After the Duodenal Switch the small bowel has two parallel limbs, the alimentary limb brings the food down from the stomach, and the biliopancreatic limb brings down the biliopancreatic secretions. These two limbs join and form the common channel.
In normal anatomy, bowel obstruction may present with nausea, vomiting, abdominal cramps, inability to pass gas, and/or have bowel movements. In this case, the X-ray will also show dilated loops of bowel and if oral contrast is given with the X-ray, there will be no contrast past the obstruction. Think of it as a garden hose that has been kinked and no water is going thru.
In this upper GI- the contrast travels down the small bowel and the entire small bowel is the same caliber. This is normal study with no evidence of obstruction. In a patient with the DS, the patient my have the biliopancreaitc limb obstruction, with an identical X-ray as above, since the oral contrast given will never get to the biliopancreatic limb and it will not show if it is dilated or not.
In duodenal switch operation, a patient may have complete obstruction of the alimentary limb, with nausea, vomiting and abdominal pain, and yet have bowel movements because the content of the biliopancreatic limb is getting to the common channel. Similarly, a patient with biliopancreatic limb may have nausea, but no vomiting, because the obstructed biliopancreatic limb is not connected to the stomach and the content can’t not be expelled from the stomach.
The images of fluid filled loops of bowel are highly suspicious.
It is critical to make sure that a patient with a suspected bowel obstruction after the DS, is evaluated with the understanding that the common signs and symptoms, and the diagnostic workup will not provide an accurate picture. A patient with the DS or RNY, can have bowel obstruction and still have bowel movement, and no vomiting.
A patient with suspected bowel obstruction should have CT scan of the Abdomen with oral and IV contrast. The cardinal findings will be “dilated loops of bowel with no contrast within the lumen of the bowel”. This is highly suspicious for bowel obstruction after DS, where the regular x ray will not pick this up. Additionally, abnormal liver function test may suggest biliopancreatic limb obstruction.
- Cheers! Alcohol Metabolism December 17, 2024
- Vitamin Toxicity December 17, 2024
- Too Much Protein & Protein Metabolism December 17, 2024
- Digestive Juices December 16, 2024
- A patient story: Lap Band complication and Wegovy October 24, 2024