Vitamin A, Absorption, and Wound Healing
September 25, 2019 8:39 am
Vitamin A is one of the 4 fat soluble vitamins along with vitamin D, Vitamin E and Vitamin K. It is multifunctional and essential which means that it is not produced by the body. In this article we will touch on aspects of Vitamin A absorption and it’s effect on wound healing as well as its metabolism.
We often think of Vitamin A as the critical vitamin for vision, however it has several other roles that related to immune function, protein synthesis, and cellular communication. Vitamin A deficiency is a concern world wide because of the natural of the side effects. Vitamin A deficiency is the leading cause of preventable childhood blindness in the world according to UNICEF and sometimes it may be undetected until there is irreversible damage.
There are 2 chemical forms of vitamin A in diet:
Retinoids (Preformed vitamin A) This group include retinol, retinyl esters, and retinal they are mostly found in animal sources like liver, egg yolk or fish oils.
Carotenoids (Provitamin A) This group includes beta-carotene, alpha-carotene and lycopene, mainly found in plant sources like leafy vegetables or yellow/orange vegetables and fruits.
The Physiology of the Vitamin A is as follows:
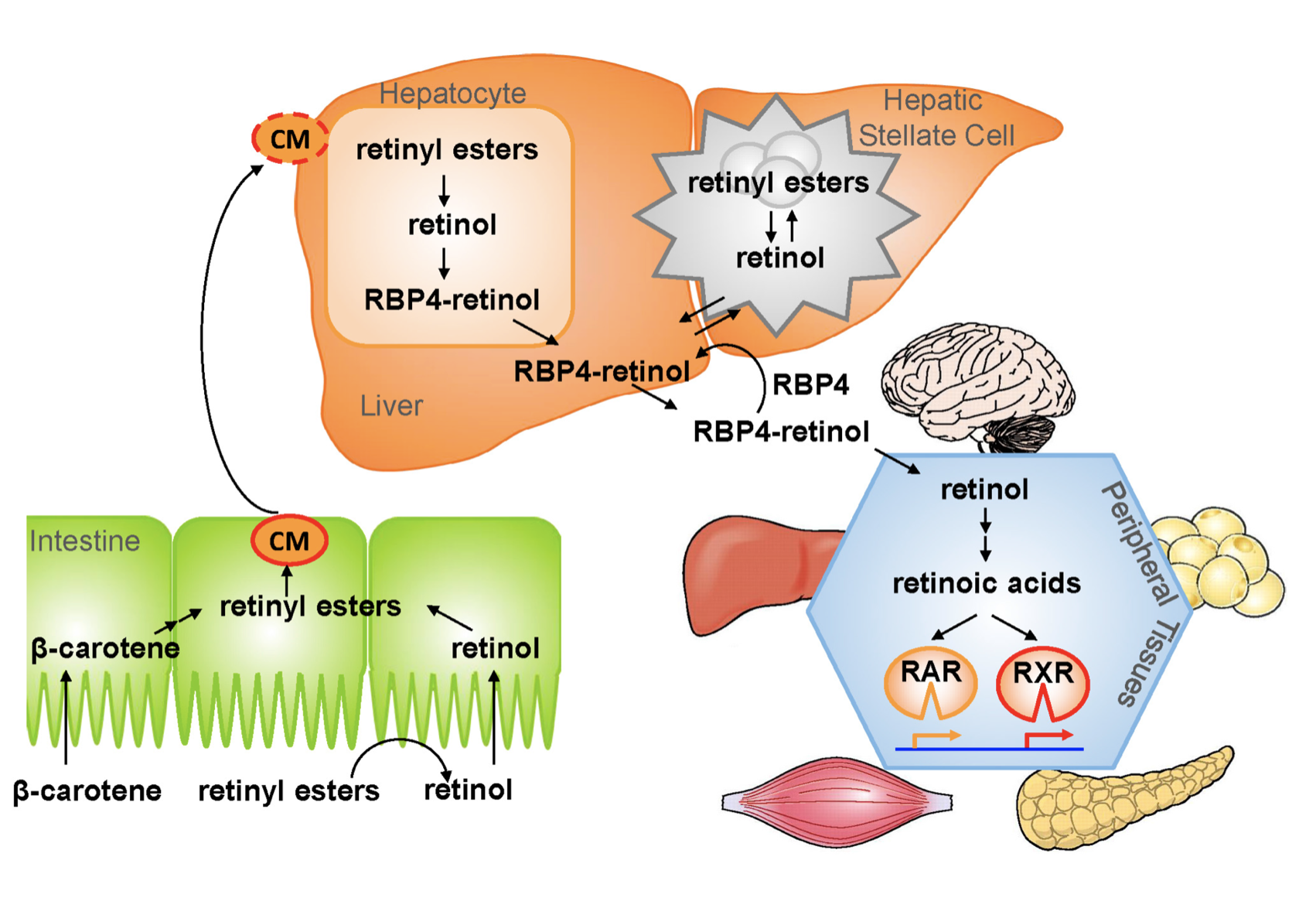
1.- Ingested food is digested in the stomach where retinyl palmitates (esters) are released from proteins. Retinol and beta-carotene are absorbed directly into the small intestine where retinyl esters and betacarotene are transformed into retinol . Retinol is the most easily absorbed form of vitamin A.
2.-That retinol absorbed by the enterocytes in the ileum (small intestine) along with bile is then transported to the liver with the help of chylomicrons a protein that transports fat.
3.-Fifty to 80% of the vitamin A is stored in the liver and the remaining is deposited into adipose tissue, lungs and kidneys.
4.-When stored retinol is released from the liver into the circulation to target organs, it is bound to plasma retinol-binding protein (RBP4) a transporting protein produced by the liver that requires ZINC, which is synthesized by the liver; This complex is stabilized by transthyretin (TTR), which reduces renal excretion.
Retinol is a crucial component for reproduction, embryological development, cellular differentiation, growth, protein synthesis, and immunity in the form of retinoic acid and vision in the form of retinal.
One of Vitamin A additional roles is in epithelial health of skin and mucous membranes. It increases epithelial turnover which is crucial during would healing. It also has anti-oxidative effects which prevent cell damage and can prevent or reverse the effects of other damaging agents. In addition to these benefits it has also been associated with increasing collagen, fibronectin, keratinocytes and fibroblast, all important in wound tissue structure. There have been some studies that suggest giving higher doses of Vitamin A in patients with non or slow healing wounds.
It is important to remember that we have documents delayed diagnosis of adult vitamin A deficiency leading to significant night blindness in adults. It is critical that the patients and their primary care physicians are acutely aware of this possibility. In majority of the patients with low vitamin A, post weight loss surgery, aggressive supplementations, including injections need to be considered as a part of the treatment regimen.
We would like to thank Miguel Rosado, MD for his significant contribution provided for this Blog.
Colonic Volvulus
September 10, 2019 11:23 am
A volvulus is when a loop of intestine twists around itself and the mesentery that supports it, resulting in a bowel obstruction that can compromise intestinal blood flow. For this reason, it tends to be a surgical emergency which requires prompt attention; failure to recognize the signs and symptoms of intestinal volvulus may lead to bowel ischemia and perforation. A volvulus can develop anywhere along the intestine, however for this blog we will discuss types of Colonic Volvulus.
The most common forms of volvulus in gastrointestinal tract is sigmoid followed by cecal volvulus, these are both colonic volvulus. Sigmoid volvulus is responsible for 80% of intestinal obstructions. High-fiber diets and chronic constipation are common risk factors because they cause increased gas and sigmoid colon elongation. Worldwide the incidence in men is much higher than in women, and this may be explained by the mesenteric shape, which tends to be longer and have a narrower base. In weight loss surgical patients specifically, such as Duodenal Switch, increased gas and diarrhea is common in those patients who have carbohydrate and fiber rich diets. In some cases, they are recommended to have high fiber diet by other providers who may not be aware that this may only be complicating the problem and exacerbating the symptoms. The solution would not include adding fiber but rather eliminating the underlying food items causing the increased gas and diarrhea.
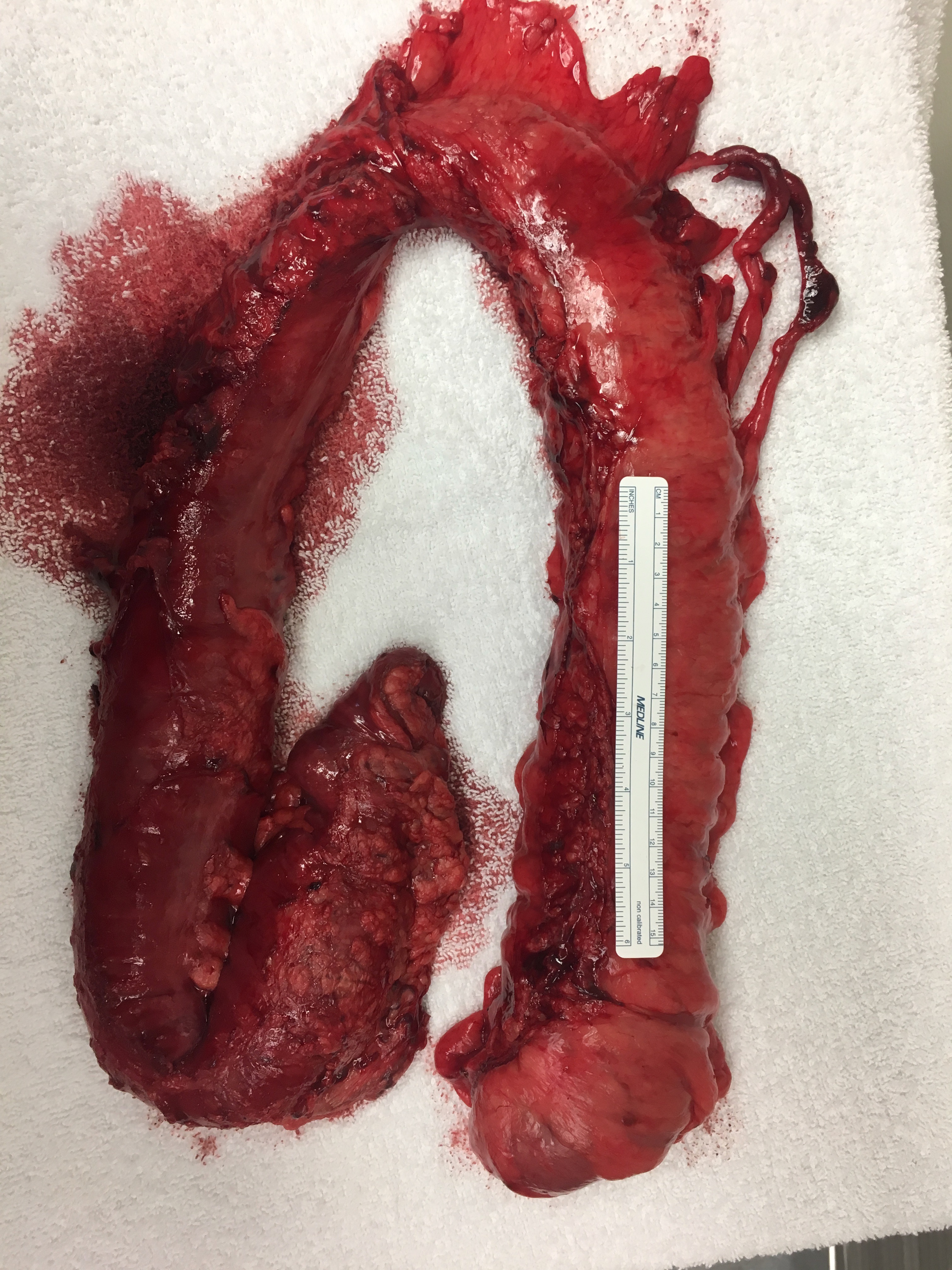 The presentation of volvulus is much the same, regardless of its anatomic site; Cramping abdominal pain, distention and constipation are present. With progressive obstruction, nausea and vomiting will occur.
The presentation of volvulus is much the same, regardless of its anatomic site; Cramping abdominal pain, distention and constipation are present. With progressive obstruction, nausea and vomiting will occur.
A definitive diagnosis is made with a CT scan, and the treatment is generally a bowel resection. However in the case of a sigmoid volvulus an urgent endoscopic detorsion may be attempted first, only if there are no signs of ischemia. The risk of recurrence following endoscopic detorsion alone is as high as 90% and carries a high risk of mortality up to 35%, therefore definitive elective sigmoid resection is recommended.
Here is a short video of an operation.
We would like to thank Miguel Rosado, MD for his significant contributions provided in this Blog.
Sleeve And Weight Regain
July 22, 2019 9:50 am
 Felsernreich et.al. demonstrated that 10 years after sleeve gastrectomy 33% were requiring revisions of their sleeve due to weight regain or reflux. 66% needed revision for weight loss and only 34% for reflux. Those patients who have revision to gastric bypass (in their practice all being revised with two exception) had resolution of their reflux however had no sustained weight loss after the revisions. This supports our position that we have had for years that the those patient who had the sleeve and are experiencing weight regain, recurrence of comorbidities inadequate weight loss ahould all be revised to the duodenal switch operation.
Felsernreich et.al. demonstrated that 10 years after sleeve gastrectomy 33% were requiring revisions of their sleeve due to weight regain or reflux. 66% needed revision for weight loss and only 34% for reflux. Those patients who have revision to gastric bypass (in their practice all being revised with two exception) had resolution of their reflux however had no sustained weight loss after the revisions. This supports our position that we have had for years that the those patient who had the sleeve and are experiencing weight regain, recurrence of comorbidities inadequate weight loss ahould all be revised to the duodenal switch operation. 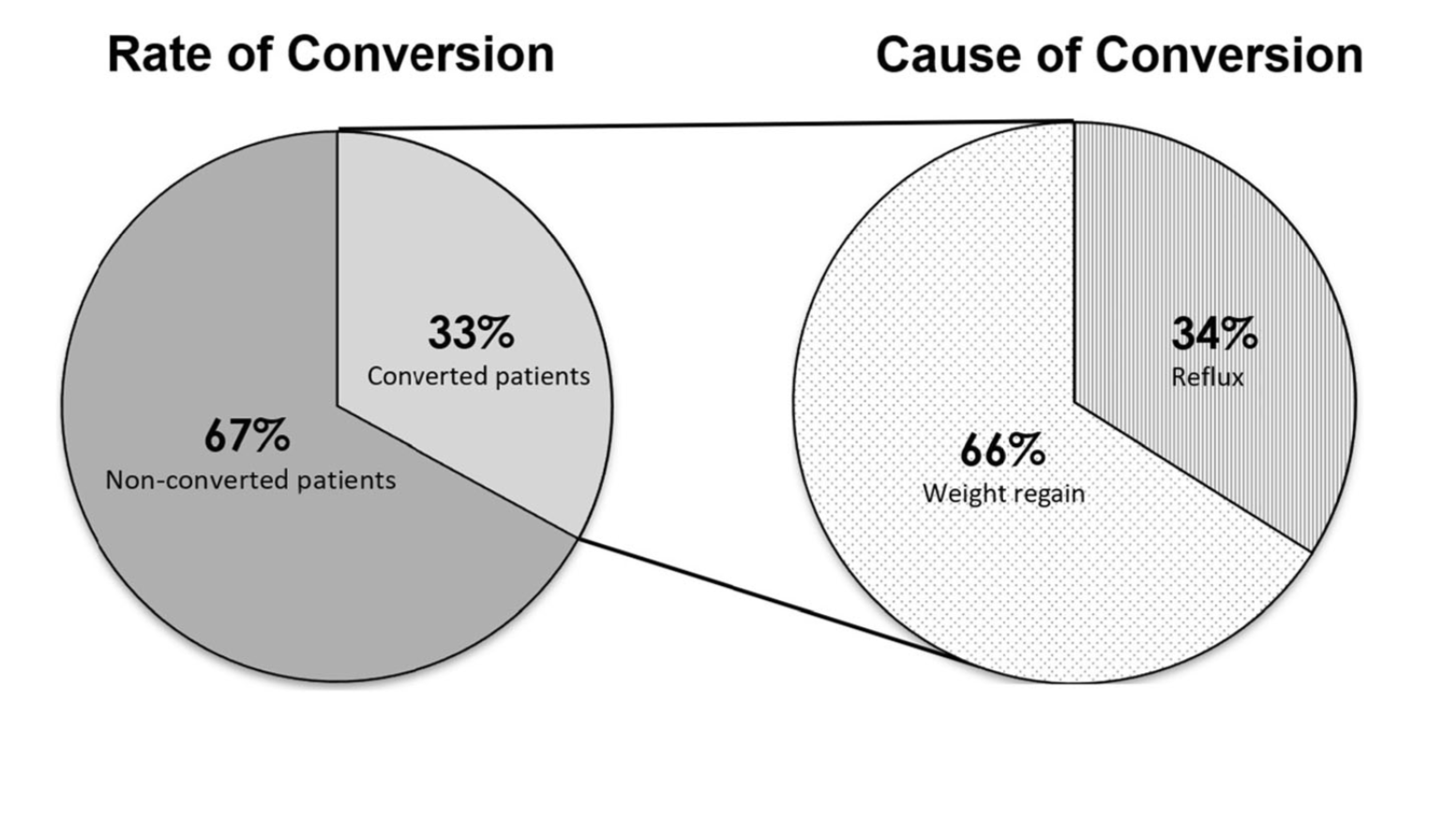
Sunscreen
June 27, 2019 3:03 am
Recently there has been some research and concern regarding sunscreen and the chemicals within them. This has led to findings that can be concerning but that need further research.
Post weight loss surgical patients, and in general patients who suffer with obesity, before or after weight loss surgery, have low vitamin D level. This may be caused by a number of factors. One such factor may be the reluctance to get skin exposed to sunlight in order for the bodies natural Vitamin D pathways functioning.
The recommendations are for daily exposure to sun. This not only is critical to the vitamin D metabolic pathways, but also help with bone health, immune function, mood, counteracting depression.
In a recently published online article, concerns were raised that some of the ingredients of some of few sunscreens are absorbed in the blood stream. This is a small study, and as the results indicates, it is not recommending to stop using the sun screens. Be aware of your sun exposure, timing exposure, and the ingredients in your sunscreen.
You can find past blog posts on Vitamin D, Bone health, etc here
Thyroid Medication Absorption And Weight Loss Surgery
June 10, 2019 8:59 am
Question : “Do I have to take higher dose of thyroid medication after the duodenal switch? ”
Answer : “Maybe”
With all weight loss surgical procedures, there may be changes to absorption of medications. It is easily understood why duodenal switch may results in decreased absorption of fat-soluble medication. What is not as clear is the reduction in absorption of other medication with procedures that do not explicitly change the absorption at the level of the small bowel directly.
The research data is all over on this topic. There is published literature that shows improvement in the thyroid function after gastric bypass and the sleeve gastrectomy. However, the exact mechanism is not completely understood.
There is research that reports “…decreased postoperative levothyroxine requirements.” Other have shows no correlation between the length of the bowel distal to duodenum to absorption of thyroid medication.
With all this confusing data, the best course would be to always “treat the patient and not the lab results.”
 If a patients who has been on medications with stable number and symptoms, suddenly presents with complaints of hypothyroidism after weight loss surgery, it’s possible the medications should be up adjusted even if the thyroid lab values may not be as defining.
If a patients who has been on medications with stable number and symptoms, suddenly presents with complaints of hypothyroidism after weight loss surgery, it’s possible the medications should be up adjusted even if the thyroid lab values may not be as defining.
Osteoporosis Medications, Action and Side Effects
May 25, 2019 3:40 pm
Treatment options should be approached is a global and systemic fashion. It is critical that the nutritional status is at its best possible and optimized for important healthy bone vitamins and minerals. Low protein needs to be corrected. Special attention should be given to nutrients, minerals and vitamins. These include Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1/K2to name a few.
Healthy bones require ongoing and routine force in the form of exercise to remain health. Just as exercise improves muscle strength, it also improves bone health. Exercise is also critical in improving bone structure and density. Ideally, exercise should be weight bearing and resistance. Examples include: hiking, walking, jogging, climbing stairs, playing tennis, and dancing. Resistance type exercise is weight lifting and resistance bands. These exercise work by creating a pull or force on the bone either by gravity, movement or weight. Always check with your physician before beginning an exercise routine, start slowly and building up to longer periods of time. The ideal goal would be at least 30 minutes a day, every day, if you are able.
We frequently see patients immediately started on osteoporosis medications without checking or improving some of the nutritional markers noted above or without looking at exercise history. In some case, the medication recommended are contraindicated due to nutritional status.
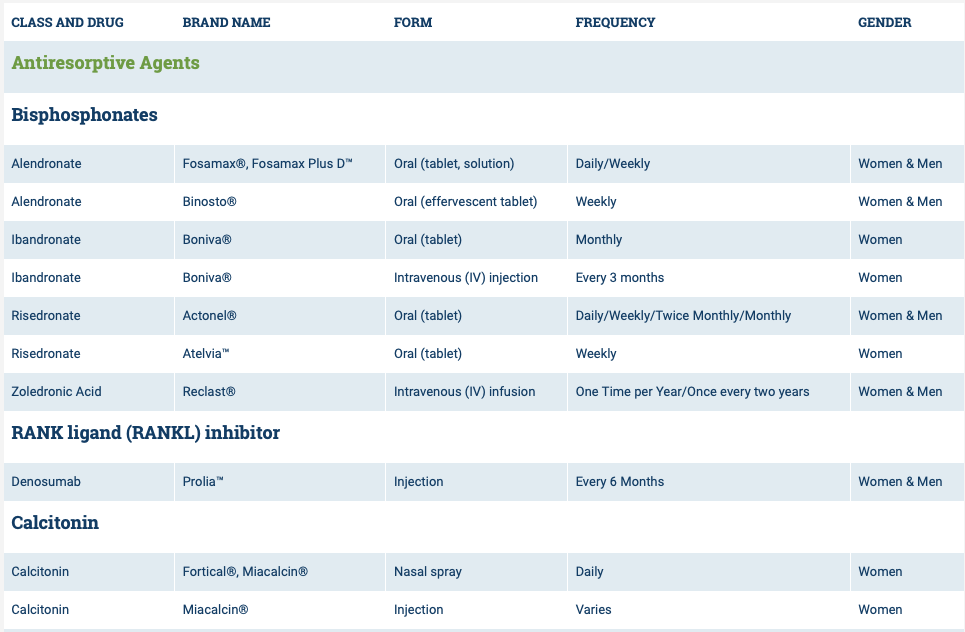
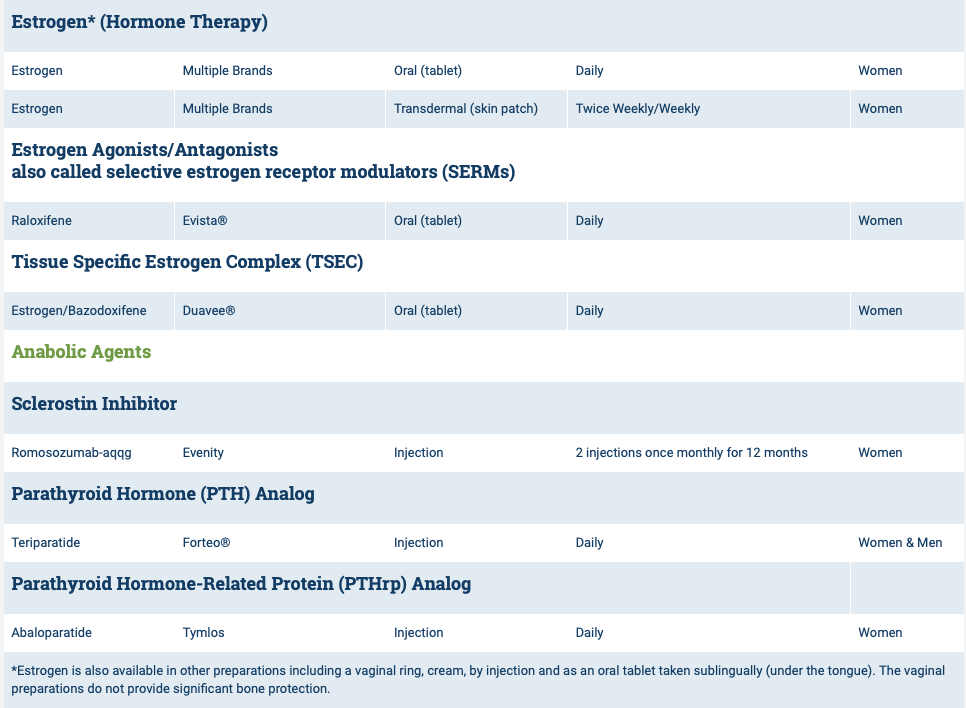
The medications can be grouped in to those that help with new bone formation (Anabolic agents) or those that help by suppressing the bone breakdown phase (Antiresorptive agents).
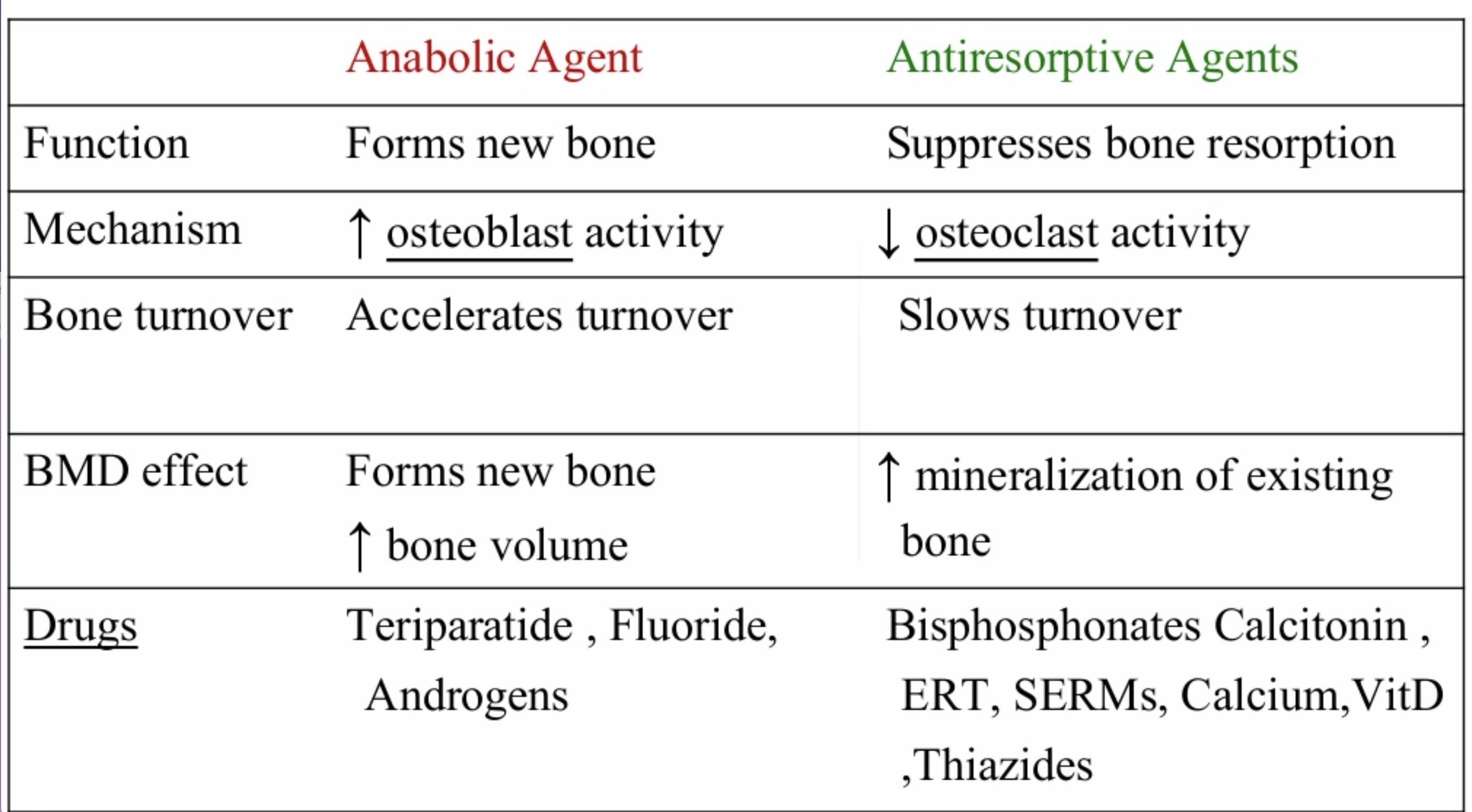
National Osteoporosis Foundation has an exhaustive list (below) of medications for treatment of Osteoporosis.
The table below outlines the side effects and mechanism of the actions of the common medications used for treatment of osteoporosis which was published by the University Health News Publication on August of 2014.
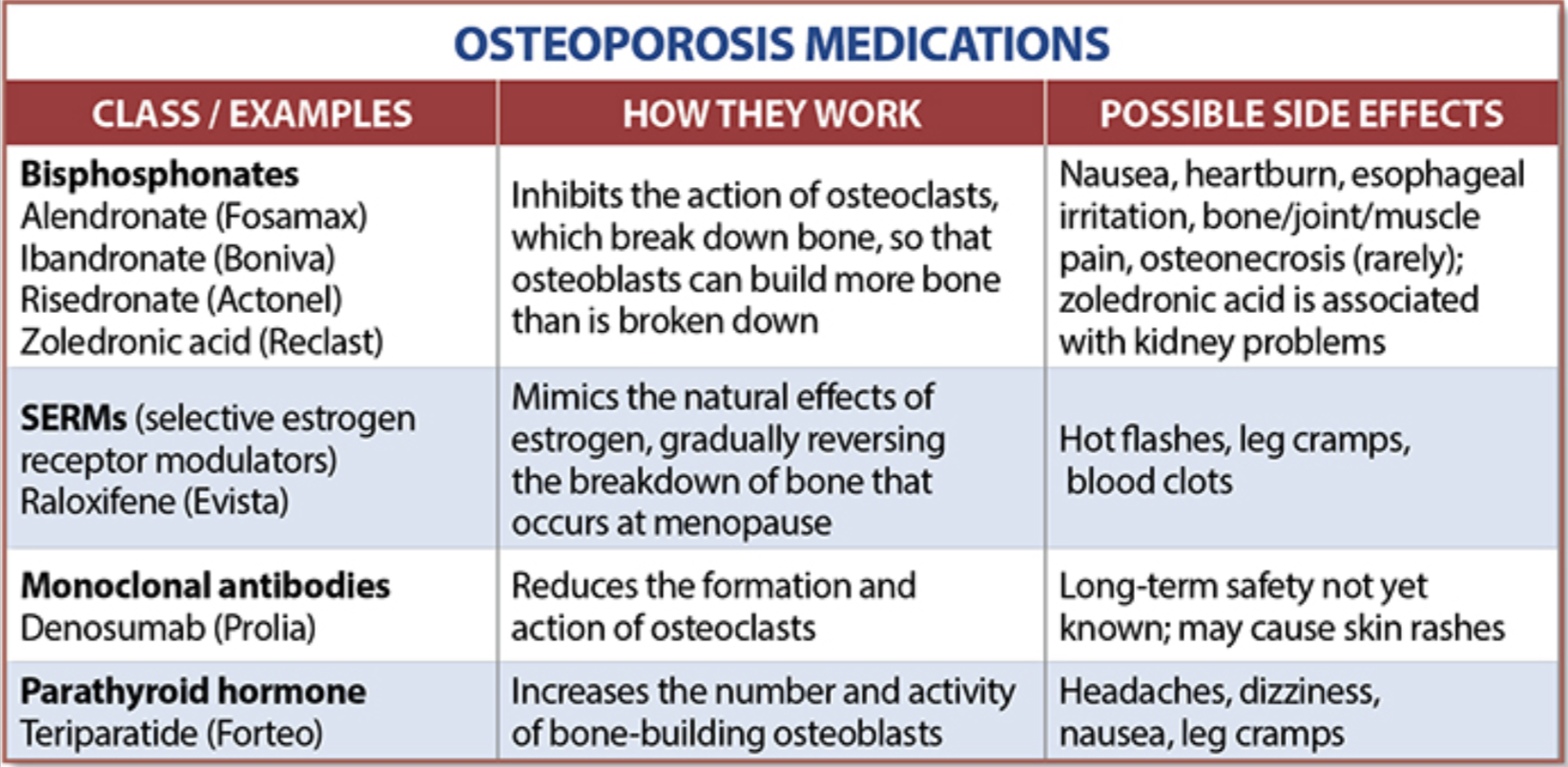
With all this information, the few points to remember is that the most important factors in healthy bone structure are the nutritional status Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1 levels.
This is an animation of normal bone Metabolism. It shows how bone structures is taken down and rebuilt continuously. This allows for a healthy bone maintainence as we age. The key is the balance of breakdown (osteoclast) and the build up (osteoblast) activity is regulated. Osteoporosis develops when there is more breakdown that build up. 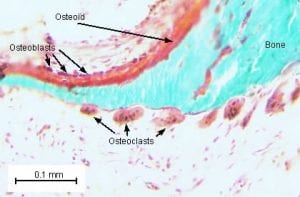
With permission of Dr. Susan Ott of University of Washington.
Additional information available on her site.
Past blogs on Bone Health.
Protein Sources
May 16, 2019 10:26 am
Not all proteins are created equally. The protein that we digest serves as the source of the essential amino acids, (the building blocks which make up a protein). The essential amino acids can not be made in out body. Protein sources can be animal or plant based. We’ve written a in-depth explanation of protein sources in this previous blog: Protein Optimization
The proteins can also be decided into two categories:
1-High quality or Complete proteins
Complete proteins contain all the indispensable amino acids that we need. Animal based proteins for the most part are complete proteins. These include cheese, mean, fish, mild, yogurt, egg and poetry.
2-Low quality or Incomplete proteins
Incomplete protein are mostly plant based proteins. In most cases, the incomplete proteins either lack or have insufficient about of the one or a number of amino acids to be able to satisfy our nutritional requirements.
This is why we general recommend animal based proteins.
Following weight loss surgery there are some guidelines that can be helpful in our previous blog: Importance of Protein.
Gastroesophageal Reflux: Bile Vs. Acid
May 14, 2019 12:52 pm
Gastroesophageal (GE) reflux is the condition when the stomach content are able to “reflux” back thru an incompetent lower esophageal sphincter (LES) into the esophagus.
Gastroesophageal reflux Disease (GERD) is the clinical condition which is the result of long standing reflux and results in microscopic and visible changes to the inner lining of the esophagus, esophageal mucosa.
GERD is a non descriptive as to the cause of the condition. It only states that the content of the stomach have been irritating the lining of the esophagus on chronic bases. This can be caused by an anatomical abnormality fo the GE junction (Hiatal Hernia), or may be related to disfunction the LES. Other possible causes of the GERD may be infection (H.Pylori) environmental (stress) and dietary (nicotine, alcohol, caffeine, spicy food) in origin.
So far we have not clarified the chemical nature of the the refluxed content.
In Acid Reflux, the relative acid overproduction of acidic secretion and the exposure of the esophageal mucosa is what needs to be addressed. This is accomplished by acid suppression medications, Anti Histamine (H2 blockers) Proton pump inhibitors (PPI) for example. The physiology, and the mechanism involving this condition is well understood. As a surgeon, we do however see patients who should have had surgical intervention. The initial mode of therapy for a patient with documented acid reflux, and or symptomatic hiatal hernia is placing them on medication. These patients are then recommended to have related upper endoscopy. Patients who do not improve or where deterioration of the esophageal mucosa, presence of precancerous cells, then the patients are referred for surgical intervention.
Bile Reflux, contrary to acid reflux may have very little if anything with the LES. The symptoms experienced by the patient may be as ofter related to the excessive bile in the stomach seen frequently
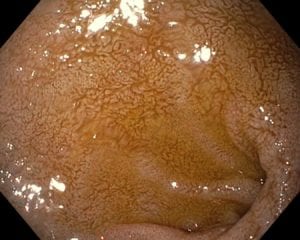
after cholecystectomy, or in those patients with dysfunctional gallbladder (low EF on HIDA scan).
The treatment of Bile reflux, is Duodenal Switch with without the associated sleeve gastrectomy component in addition to repair of hiatal hernia if present Ann Surg. 2007 Feb; 245(2): 247–253.
Vitamin K1 & K2, Interaction with Anticoagulant
May 11, 2019 6:00 am
During a recent group meeting, questions were raised regarding supplementing with Vitamin K1 or Vitamin K2 along with anticoagulant treatment. The table below provides a generalized summary of the Vitamin K1 and K2. The forms of Vitamin K in dietary supplements may differ depending on the supplement and the choice of the supplements may affect their absorptive behavior. This creates a challenge in regulating lab values, especially in patient who require anticoagulation therapy. 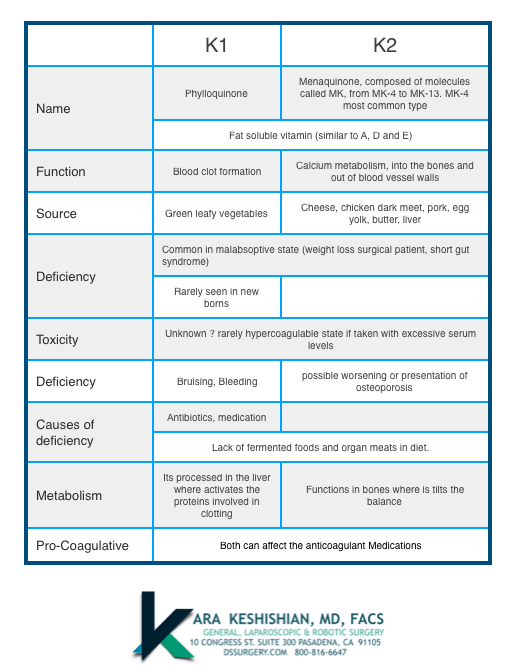
There is a lot of evidence that distinguishes between the vitamin K1 and K2 and their respective function with Cognition , Skeletal Muscle Energy Metabolism and the flexibility of the arterial wall.
In summary K1 and K2 counteract the function of the anticoagulant medications. You should consult the physician prescribing the anticoagulant before taking any vitamin K1 or K2. Even as we think of K2 having less to do with coagulation pathways, it is recommended that the patients do not take any vitamin K supplements unless cleared by their physician, since K2 may also affect the anticoagulation treatment. As a patient who is prescribed anticoagulation treatment you should make your prescribing physician aware of ANY changes in your medications or supplements either over the counter or prescribed.
Sleeve Gastrectomy Failure
May 07, 2019 12:53 pm
Sleeve gastrectomy (SG) is the most commons performed weight loss surgery in the US. There is a subset of patients for which Sleeve Gastrectomy will be inefficient/ineffective. Sleeve Gastrectomy failure may be defined as inadequate weight loss or weight regain. However, in some cases this may also include non resolution of some of the co-morbidities of obesity, and/or recurrence of others.
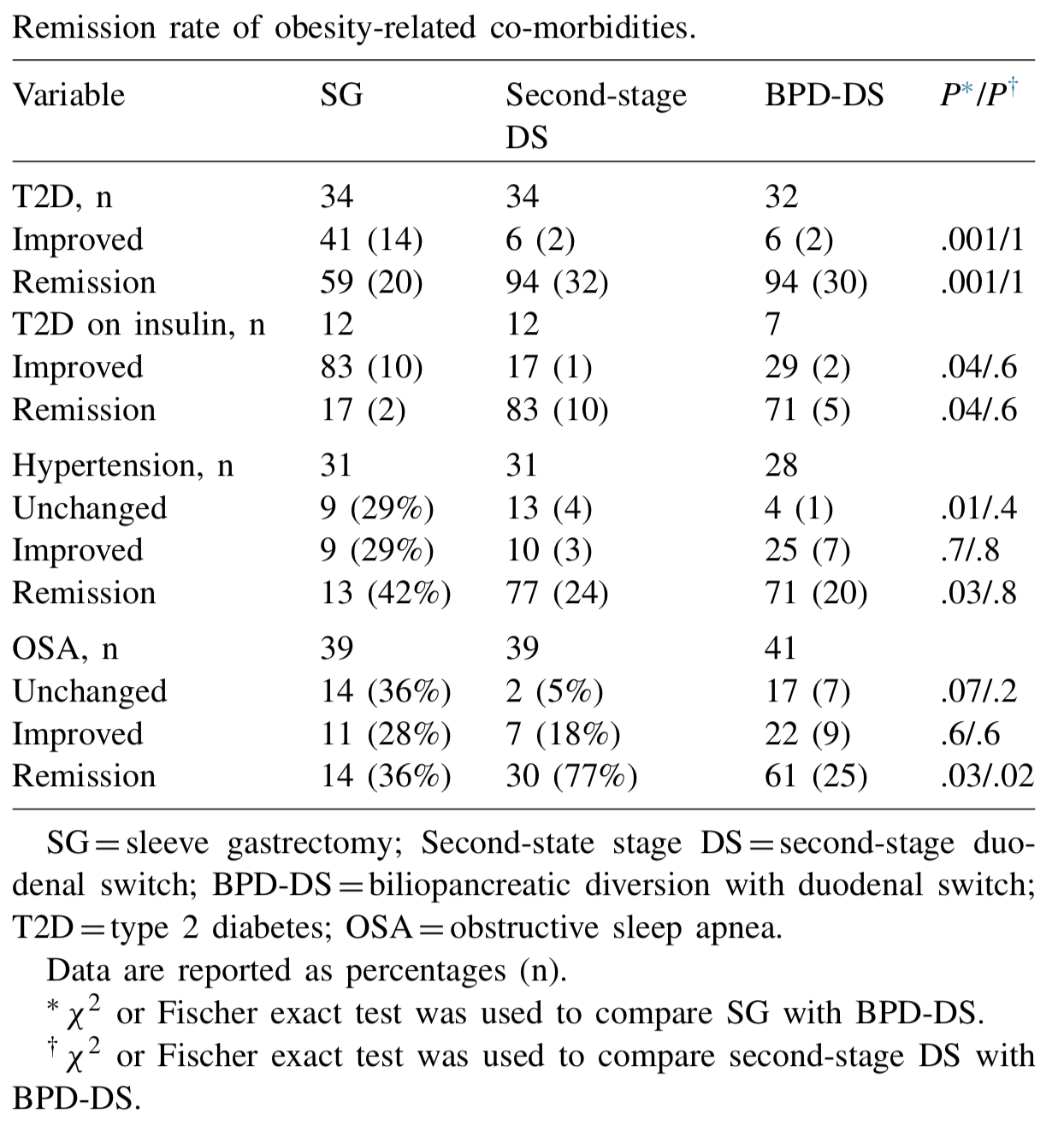
Biertho, et. al, (Surgery for Obesity and Related Diseases 14 (2018) 1570–1580) Published a study titled “Second-stage duodenal switch for sleeve gastrectomy failure: A matched controlled trial” where 118 patients were decided in two groups. One group had the duodenal switch as a singe procedure, and the second group had the sleeve gastrectomy followup by the second stage duodenal switch. They concluded that “Second-stage DS is an effective option for the management of suboptimal outcomes of SG, with an additional 41% excess weight loss and 35% remission rate for type 2 diabetes. At 3 years, the global outcomes of staged approach did not significantly differ from single-stage BPD-DS; however, longer-term outcomes are still needed.”
They showed that the remission rate of the obesity related co-morbidities were improved.
The weight loss rate that had stopped, or in some cases where weight gain had been noted, were both reversed where by at at average of 24 months after addition of the DS to the SG patients would experience additional 39% Mean excess weight loss. 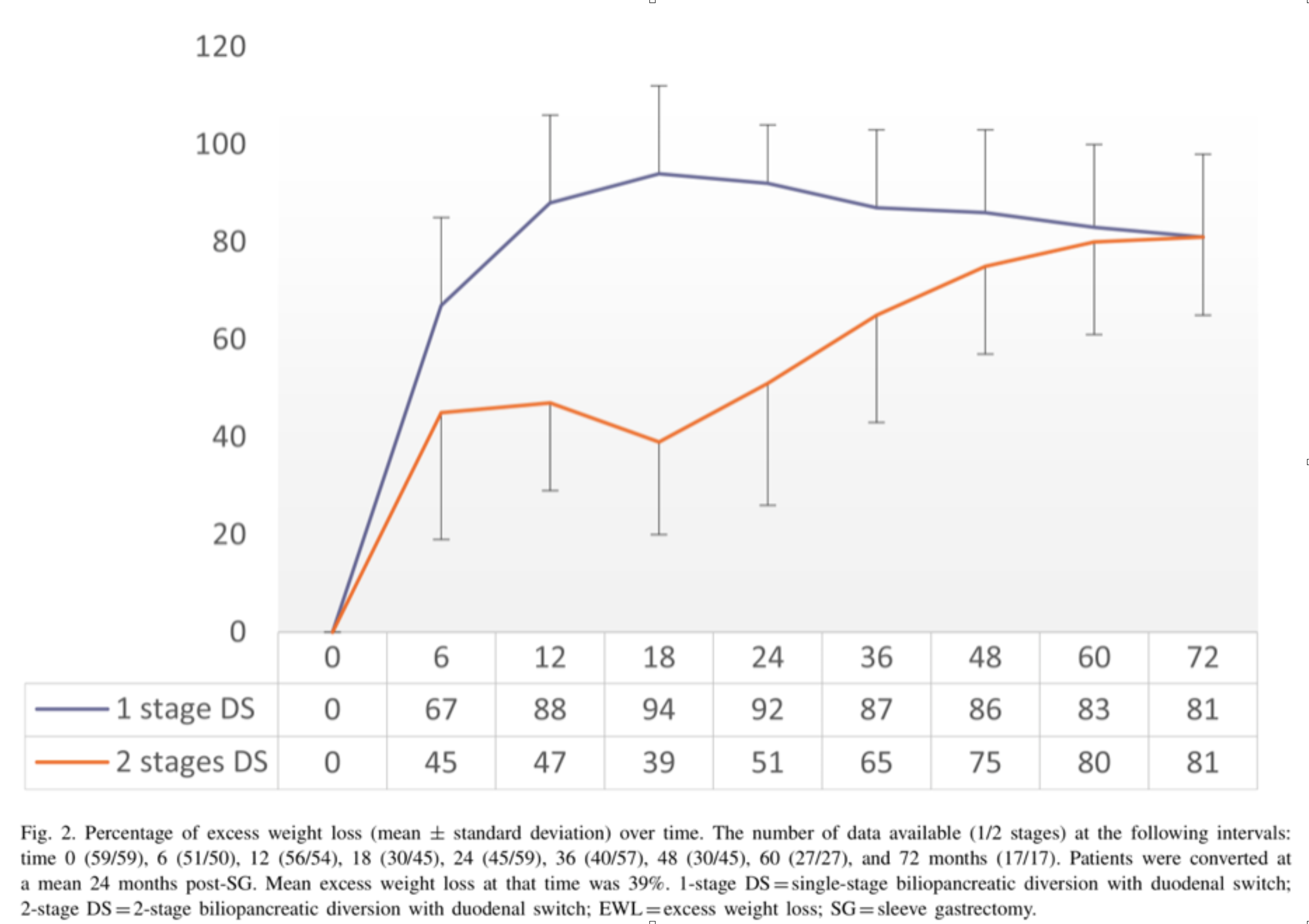
With regards to alternative approaches they indicate “ Other forms of revisions have been described, (i.e., adjustable or nonadjustable gastric band, plication, endoscopic balloon), with limited scientific evidence on their efficacy or safety. These procedures are mostly considered investigational and should be performed under Ethical Review Board approved protocols.”
In summary, patients may be offered a number of alternative if they are experiencing weight regain, inadequate weight loss, or return of co-morbidities after sleeve gastrectomy failure. We have seen a variety of them in our office. Patients who have had band placed on the sleeve, or are scheduled to have gastric balloons placed. As I have always said, buyers beware and know your outcomes and resolution of co-morbities.
Duodenal switch operation, (not the single anastomosis look alike) results in sustained weight loss and resolution of the co-morbidities. A second stage Duodenal Switch can mean adding the intestinal procedure to an existing Sleeve Gastrectomy. Some patients have required an adjustment to their Sleeve Gastrectomy in addition to adding the Duodenal Switch intestinal portion. Finding the right balance for each patient is a crucial part of our practice.